Document Type
Description
The document type dictionary is one of the most used dictionaries in Enterprise EHR. It is where an admin user can create all types of notes (documents, v10, v11, scanned documents, etc). Note properties can also be established from this dictionary.
Document Type Screenshot:
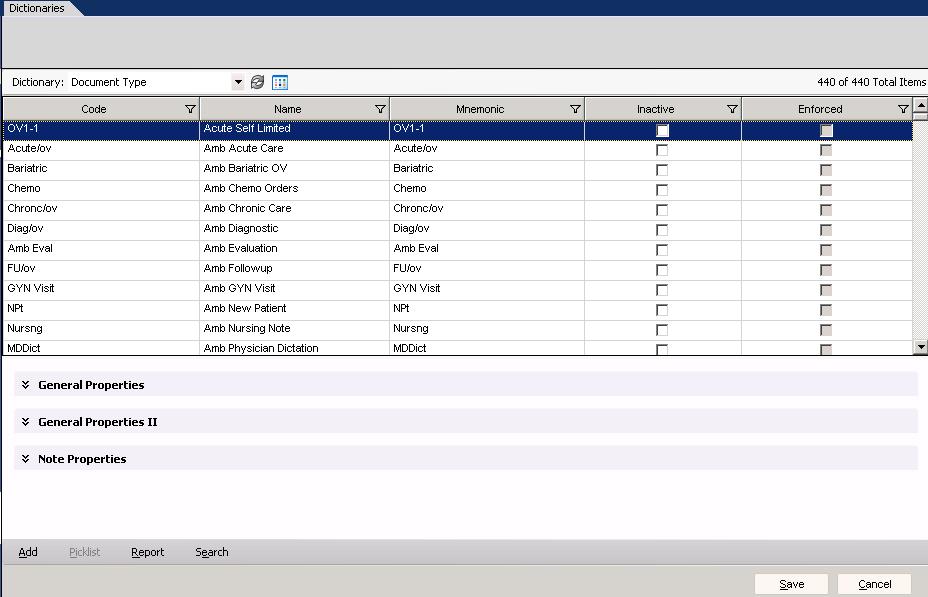
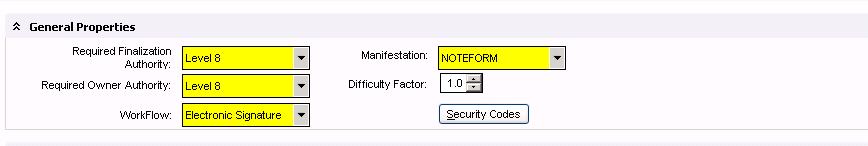
General Properties:
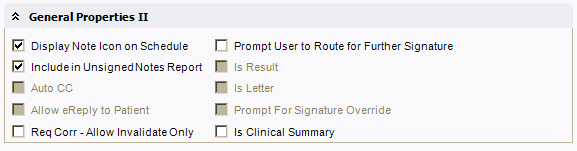
General Properties II:
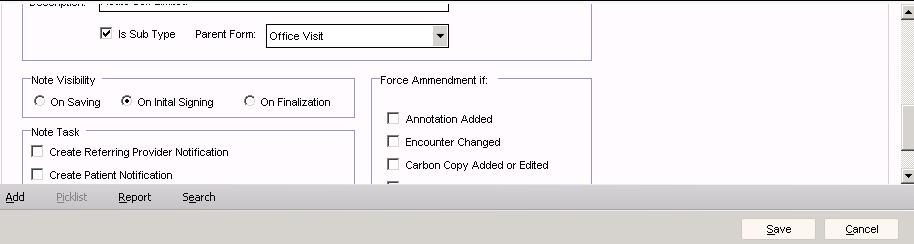
Note Properties:
Definition
Here are definitions of all possible settings contained within the document type dictionary:
General Properties
- Required Finalization Authority - This is a drop-down that indicates the level of authority that is required to finalize the document.
- Required Owner Authority - This is a drop-down that indicates the level of authority that is required to be an owner of the document.
- Workflow - This is a drop-down that determines if a document is to be verified or not. This setting should not be changed once set initially.
Electronic Signature (ES) = Documents are signed or authenticated using a unique identifier specific to the user in Enterprise, rather than a pen. This is done with the user authentication occurring through re-entry of a user password or biometric authentication.
Electronic Verification (EV) = An alternative form of authenticating documents within Enterprise without using a pen. EV is used to verify that a user has reviewed a document but is not responsible for the accuracy of its content.
Non Electronic (NONEW) = No form of electronic authentication needed, or possible since signature or verification is done outside the Enterprise EHR system by printing the document and signing using a pen.
- Manifestation - Defines the type of document.
FRM = Admin Form
HTML = v10 Structured Note
NOTEFORM = v11 Structured Notes
RTF = Unstructured Document
RTFXML = Used only for Clinical Exchange Documents (CED)
TIF = Scanned Documents
Allscripts Clinical = Allscripts Clinical Note
- Difficulty Factor - Used to indicate the level of difficulty (due to accent, subject matter, or workflow) that is associated with transcribing this document type. This is useful in Line Count reports for transcriptionists. It must be set to a value from 1.0 to 9.9; default is 1.0.
- Security Codes - Used to view or assign security codes to the document type. Delivered codes are Doc Change and Doc Change Shared. Additional codes can be manually created in Security Admin.
General Properties II
- Display Note Icon on Schedule - This should be clicked for documents that will be created relating to visits. Scanned documents usually are not checked but HTML, NOTEFORM, and RTF usually would be.
- Include in Unsigned Notes Report - This checkbox determines if this document type will be included in the Unsigned Notes report or not. It is recommended to check this box for Dictate document types.
- Auto CC - This checkbox determines if this document type can automatically be carbon copied.
- Allow eReply to Patient - Indicates whether or not a document can be used to reply to Patient online (user must also have eReply security code).
- Prompt user to route for further signature - when checked, this will display a dialog box prompting the signing user to route to a second user to co-sign the document. This is typically used for resident or mid-level provider co-signing workflows. Note that this option only works when the initial signer does NOT have sufficient authority to finalize the document AND the option must be checked at the document type, input/output level.
- Is Result - This indicates whether to flag scanned document types as a result within Chart Viewer.
- Is Letter - Indicates whether to allow users to create letters derived from notes with a suitable salutation and closing (V10 Note Only).
- Prompt for Signature Override - Allows users to override the necessary signature authority specified for the document type.
- Is Clinical Summary - Applies to v10 and v11 Note and allows a note output to be considered as a clinical summary
- For more information on Clinical Summaries, refer to our Patient Summaries page
Note Properties
- General Description - This is a text box for the description of the note. The user will see this on the front end and typically this field is the same as the display name.
- Is Sub Type - When checked, this indicates that the document type is a sub type of a parent document type.
- Parent Form - This is a drop-down list that indicates the parent document type that the document type is tied to. When this field is populated, the "Is Sub Type" field in Enterprise is automatically checked.
- Finalize Note on Save - This checkbox will determine whether or not the note automatically falls into a "Final" status when upon initially saving it.
- Note Visibility - This setting only applies to v11 notes (NOTEFORM manifestation). It does not apply to v10 structured (HTML manifestation) or unstructured notes (RTF manifestation). There are three options:
- On Saving: indicates that the output template(s) will be visible in chartviewer upon initial saving.
- On Initial Signing: indicates that the output template(s) will be visible in chartviewer upon initial signing.
- On Finalization: indicates that the output template(s) will be visible in chartviewer upon finalization.
- Note Task - This will send a delegated task to the note owner indicating that one of the following should be notified:
- Create Referring Provider Notification - Create a delegated task assigned to the note owner that the referring provider should be notified.
- Create Patient Notification - Create a delegated task assigned to the note owner that the patient should be notified.
- Create Review Covered Note Task on Finalization - Create a task for the appointment encounter provider to review the note that was finalized by the covering physician.
- Create Task on Amendment - Creates a task assigned to the note owner to sign the amended note.
- Force Amendment If - This controls whether to change the note status to Amended when one of the following events occur:
- Annotation Added - The note status will change to Amended when an annotation is added.
- Encounter Changed - The note status will change to Amended when the encounter that the note is linked to changes.
- Carbon Copy Added or Edited - The note status will change to Amended when a carbon copy recipient is added or edited.
- Note Owner Changed - The note status will change to Amended when the note owner is changed.